Parkinson's disease
| "Parkinson's is my toughest fight. No, it doesn't hurt. It's hard to explain. I'm being tested to see if I'll keep praying, to see if I'll keep my faith. All great people are tested by God." – Muhammad Ali |
|
| In continuation of my previous post about neurodegenerative diseases, today I will talk about Parkinson’s disease (PD). PD is the second most common neurodegenerative disorder, after Alzheimer's disease (AD), that affects the central nervous system. Clinical manifestations of this complex disease include motor impairments such as resting tremor, slowness of movement, postural instability, and impaired balance and coordination. These abnormalities can be accompanied by other symptoms, such as depression, and a general slowing of intellectual processes. | |
| As dopamine regulates all forms of movement, the motor symptoms of PD result from the death of dopamine-generating cells in the substantia nigra, a region in the midbrain1. By the time of death, it is estimated that this region of the brain loses 50–70% of its neurons compared to the same region in unaffected individuals! PD affects approximately seven million people globally and one million people in the United States. Most individuals with PD are over the age of 60, but early-onset PD can also occur2. | |
| PD was first described in 1817 by an English doctor named James Parkinson after he observed paralysis in six patients. However, it wasn't until the 20th century that most of the extensive studies were conducted, shedding light on the underlying biochemical changes in the brain associated with this disease. In 1912, Frederic Lewy described microscopic particles in affected brains, later named Lewy bodies, and α-Synuclein was found to be the main component of Lewy bodies in 1997. | |
| Lewy bodies and Lewy neurites are the pathological hallmark of PD3. They are abnormal aggregates of protein that develop inside the cytoplasm or the neurite of neurons. Protein aggregation can occur due to several reasons, including genetic risk factors, environmental factors, and aging. Lewy bodies appear as spherical masses that displace other cell components, and they are identified only during histological examination of brain tissue. A Lewy body is composed mainly of the protein α-Synuclein associated with other proteins, such as ubiquitin, neurofilament protein, and Alpha β crystallin4. Tau proteins may also be present, and Lewy bodies may occasionally be surrounded by neurofibrillary tangles. | |
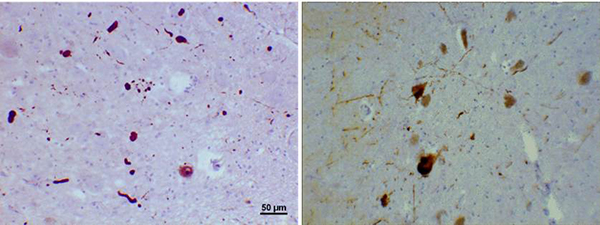 20x magnification of immunohistochemical images of regions of substantia nigra in this Parkinson's patient show rounded Lewy bodies and strand-like Lewy neurites. |
|
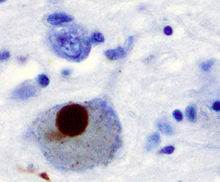 Immunohistochemical staining of a Lewy body in a brain cell of the substantia nigra in Parkinson's disease . The brown colour is positive immunohistochemistry staining for alphα-Synuclein. |
α-Synuclein (α-Syn) is a protein that is abundant in the human brain and is predominantly found at presynaptic terminals5. It belongs to the Synuclein family that also includes β-Syn and γ-Syn. α-Syn is a soluble, natively unfolded protein under physiological conditions, and it is thought that the normal function of this protein is regulation of membrane vesicle trafficking. However, missense mutations and post-translational modifications including glycosylation and nitration contribute to aggregation of α-Syn. The aggregation and accumulation of these abnormal α-Syn proteins in dopaminergic neurons have been postulated to be responsible for the subsequent neurodegeneration that is present not only in autosomal dominant early-onset PD, but also in the classical form of PD and in other CNS disorders, called α-Synucleinopathies, which include Alzheimer’s disease and Lewy body dementia. |
| Besides aggregation of α-Syn, identification of mutations in several other genes have been found which link genetic causes to PD6. Although gene defects in ubiquitin C-terminal hydrolase like 1 (UCH-L1), Parkin (PRKN), LRRK2, PINK1 and DJ-1 are responsible for only a small number of patients with PD, their identification and the proteins that they encode for are providing significant insight into the disease mechanisms that may be responsible for PD and other neurodegenerative diseases. Recent studies are also revealing a pathogenic role for oxidative stress and mitochondrial dysfunction in causing PD7. Further, environmental factors such as exposure to pesticides and aging are also known contributors of this disease. | |
| PD is usually diagnosed from the medical history of the patient and from a neurological examination. However, brain scans such as MRI and CT scans usually appear to be normal in patients with PD, and there is no medical test that can clearly diagnose this disease. PD can only be conclusively diagnosed through an autopsy of the midbrain to find Lewy bodies. In addition, there is no cure to PD, but medications, surgery, and disease management can provide some relief to these patients. For example, several treatment options are available that use dopamine agonists to induce dopaminergic stimulation, and/or use small molecule inhibitors to increase the level of dopamine in the basal ganglia by blocking its metabolism. However, to obtain better and more effective treatment options, researchers are actively pursuing studies through developing new animal models of the disease and exploring strategies such as gene therapy, stem cell transplants and neuroprotective agents. Please let us know if you have any suggestions or experience with PD research at tech@biolegend.com. | |
| Contributed by Mohar Chattopadhyay, PhD. | |
References:
|
|
 Login / Register
Login / Register 






Follow Us